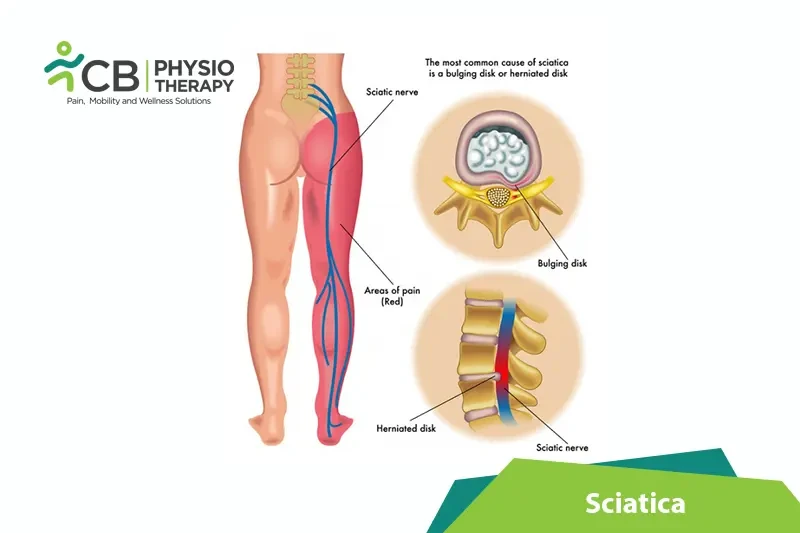
Sciatica or sciatic pain radiates along the path of the sciatic nerve, which branches from the lower back through the hips and buttocks and down to each leg. Usually, sciatica affects only one side of the body. Sciatica occurs due to a herniated disc, bone spur on the spine, or narrowing of the spine compressing the nerve, resulting in inflammation, pain, and numbness in the leg.
Any condition that compresses the sciatic nerve may cause sciatica symptoms. Commonly the reasons can be:
The symptoms of sciatica are pain due to irritation of the sciatic nerve. The type of pain can vary from person to person:
Pathology:
Sciatica occurs most commonly when a spinal nerve is compressed by a disc bulge, disc herniation, or bony spur. It causes pain, inflammation, and numbness in the affected leg. Sciatica can be severe, though most cases are resolved by non-operative treatments in a few weeks.
Physical examination:
The examiner checks for the source of the pain and discomfort. Examines the muscle strength and nerve functions, and whether the pain is felt while moving or touching the affected area. The aggravating and relieving factors are also noted along with the medical history.
Straight leg test:
A straight leg test is performed by asking the patient to lie in the supine position, then lift the leg, flex at the hip joint, and keep the knee in full extension and straight. Usually, the pain that is reproduced between 30 to 70 degrees of hip flexion and experienced primarily in the back is likely due to a lumbar disc herniation.
X-rays:
The X-ray can be done to show any bony problem and thus rule out other conditions with similar symptoms
Magnetic resonance imaging (MRI):
A magnetic resonance imaging (MRI) scan can also be done to show the location of the disk and the affected nerves.
Discograms:
A discogram involves injecting dye into the center of the disc, which helps to show cracks in the disc. It also shows whether the herniated disc is exerting any pressure on the spinal cord and nerves.
Myelogram:
A myelogram is done by injecting dye into the spinal fluid and then an x-ray image is taken.
Medications: Anti-inflammatory, Analgesics, Muscle relaxers, Opioids, Anticonvulsants, Corticosteroid injections, etc.
Note: Medication should not be taken without the doctor's permission.
Surgery:
In patients, where pain doesn't subside for a prolonged period, surgery is recommended to relieve the pressure from the nerve endings. Surgical evaluation and correction of any structural abnormalities such as disc herniation, epidural abscess, epidural tumor, or hematoma are recommended.
Cryotherapy or ice therapy is applied to decrease spasms, inflammation, and pain.
Thermotherapy or heat therapy promotes blood flow and removes toxins.
Lumbar support:
Lumbar support is used for short-term support to limit the movement of the lower back.
Massage therapy like deep tissue massage helps to improve blood circulation and decrease inflammation.
Ultrasound uses sound waves, that stimulate the affected area and improves blood flow to the affected part.
Transcutaneous electrical stimulations (TENS):
Transcutaneous electrical stimulations (TENS) promote gentle relaxation and decrease pain.
Interferential therapy is also recommended to reduce pain and inflammation.
Traction:
Traction reduces the weight on spinal discs, alleviates pressure on the affected nerve, and relieves pain.
Laser therapy is another advanced electrical modality that enhances the healing process, decreases pain, and increases mobility.
Manipulation and mobilization:
Manipulation and mobilization, both techniques are used to break the adhesions, align the bones and improve mobility.
Strengthening and stabilization exercises:
These exercises include exercises to increase core muscle strength and support for the back. Back strengthening exercises are done for the trunk and all layers of the core muscles, which helps to support the low back and prevent excessive strain through the discs.
Stretching exercises:
Gentle stretching of the lumbar spine and hamstrings are done to improve the flexibility of the back muscles.
Hydrotherapy:
Regular light exercises like doing simple range of motion exercises in water, walking in water, and swimming, are beneficial.
Balance exercises:
Balance exercises are taught to train the patient to show how the back should be while moving during various activities.
The patient is advised to avoid activities or prolonged sitting/standing and to practice good, erect position. Avoid lifting heavy objects, sudden twisting, and turning movements that lay stress on the back.
Select your City to find & connect with our experts regarding Physiotherapy for Sciatica