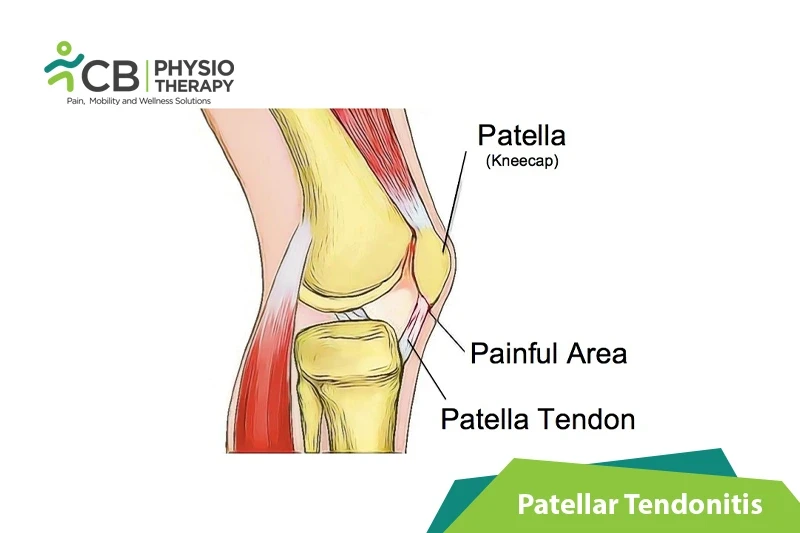
Patellar tendonitis or jumper's knee is an injury that occurs to the patellar tendon which connects the patella to the shinbone. The patellar tendon works with the muscles at the front of the thigh to extend the knee, while kicking, running, and jumping, without it, we cannot straighten the knee or jump. The patellar tendon is actually a ligament as tendons connect a muscle to a bone and ligaments connect two muscles. The patellar tendon provides stability and holds the bones together.
Patellar tendonitis occurs when the patellar tendon tissue becomes swollen or irritated. Certain factors that can cause patellar tendonitis are:
Patellar tendonitis may cause minor to severe pain which worsens over time. The condition becomes debilitating if left untreated. Symptoms of patellar tendinitis include:
If patellar tendonitis is not treated, a person may have a risk of tendon tear. A large tear of the patella tendon is a serious injury, and a complete tear separates the tendon from the kneecap. The person may hear a tearing or popping sound with significant pain.
Pathology
Patellar tendinitis is an overload lesion. Its pathology reveals focal degeneration and micro-tearing at areas near the insertion of the quadriceps or patellar tendon.
Physical examination:
Physical examination includes evaluation of the symptoms. Palpation of the patellar tendon knee to check where it hurts. In case of patellar tendonitis, pain occurs on the front part of the knee, just below the kneecap. Pressure is applied to the parts of the knee to determine where it hurts. To evaluate the range of motion patient is asked to gently move the knee in different directions, and the results are recorded.
X-ray:
X-ray is used to rule out the other causes of pain around the kneecap. It can help to exclude other bone problems that can cause knee pain.
Ultrasound:
This test uses sound waves to create an image of the knee, revealing tears in the patellar tendon. It can be used to observe structural damage to the patellar tendon.
Magnetic resonance imaging (MRI):
Magnetic resonance imaging (MRI) uses a magnetic field and radio waves that create detailed images of the subtle changes in the patellar tendon.
Medication: NSAIDs, corticosteroids, pain relievers such as ibuprofen or naproxen sodium, etc.
Note: Medication should not be taken without a doctor's prescription.
SURGICAL AND OTHER PROCEDURES
If conservative treatments don't relieve symptoms, then other therapies are required, such as:
Corticosteroid injection: It is an ultrasound-guided corticosteroid injection aimed into the sheath around the patellar tendon, which may help to relieve pain. But this can also weaken tendons and make the tendon more prone to rupture.
Platelet-rich plasma injection: This type of injection can be done in people with chronic patellar tendon problems. These injections might promote new tissue formation and also help to heal tendon damage.
Oscillating needle procedure: This procedure is performed using local anesthesia. Doctors use ultrasound imaging to guide a small oscillating needle that cuts away the damaged area.
Surgery: In case other treatments fail, surgical debridement of the patellar tendon procedures can be done, through small incisions around the knee.
Rest:
Rest is recommended as it gives the body time to heal.
Cryotherapy helps to decrease swelling around the knee, Ice is applied on the area for 15 minutes, a few times a day.
Knee brace:
A knee brace is recommended to support the knee, these devices help to relieve the pain.
Patellar tendon strap:
This strap applies pressure to the patellar tendon that helps to distribute force away from the tendon and directs it through the strap and thus helps relieve pain.
Therapeutic ultrasound:
Therapeutic ultrasound accelerates tendon healing, augments tendon repair, and modulates tendon cell activity.
Transcutaneous electrical stimulation (TENS):
Transcutaneous electrical stimulation (TENS) is an effective electrical modality that helps to decrease pain and inflammation.
Laser therapy can help to accelerate tissue repair and cell growth causes faster-wound healing, reduces fibrous tissue formation, and increases repair and regeneration. It also helps to decrease inflammation and pain.
Shock wave therapy uses sound waves to heal the tendon and thus enhance the healing process.
Iontophoresis:
Iontophoresis involves spreading a corticosteroid medicine on the skin and then using a device that delivers a low electrical charge to push the medication through the skin.
Stretching exercises:
Stretching exercises can help reduce muscle spasms and lengthen the muscle-tendon unit. While performing the stretching exercises patient should not do a bouncing movement. These movements slowly increase the strength and flexibility of injured tendon tissues. More elastic tissue is less likely to tear thus stretching should be done regularly to make the muscles and tendons more elastic. E.g. Seated hamstring stretch, quad stretch, squats, supine leg lifts, etc.
Strengthening exercises are done for weak thigh muscles which contribute to the strain on the patellar tendon. Exercises involve lowering the leg very slowly after extending it, this exercise can be helpful, as they strengthen all the leg muscles in combination, such as a leg press.
Balance and proprioception exercises:
Balance and proprioception exercises are important in case the patient feels instability while walking. This can be achieved by recommending exercises to improve proprioception and stability.
A proper warm-up should be done to give muscles time to wake up, which makes injury less likely. The patient should not do wrong exercises, as doing too much too soon, can cause further damage. Proper technique in takeoff and landing in sport should be used. The patient should be careful while doing gentle exercises and progress slowly. Activities or movements that trigger the symptoms should be avoided and further pushing through pain may cause more damage to tendon tissues.
Select your City to find & connect with our experts regarding Physiotherapy for Patellar Tendonitis