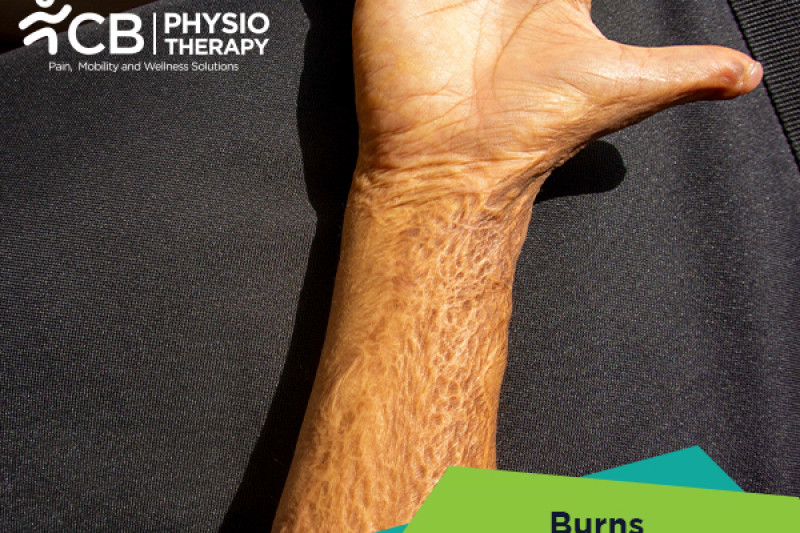
Burns are injuries that cause damage to the skin and the underlying tissue by heat, chemicals, electricity, radiation, or sun. This damage resulting from burns can be minor or even life-threatening, depending on the intensity of heat, the total area of tissues burned, and the length of exposure to the skin.
Degrees of burns:
There are different degrees of burns. The degree of a burn is based on the amount of skin affected and the depth of the burn.
First-degree burns:
First-degree burns are mild involving the outermost layer of the skin, called the epidermis e.g. sunburns. The top layer of skin turns red and painful but without the formation of blisters.
Second-degree burns:
Second-degree burn causes damage to the second layer of skin, known as the dermis. This burn causes pain, redness, swelling, and blistering.
Third-degree burns:
Third-degree burns affect all three skin layers i.e. epidermis, dermis, and hypodermis. The burn also destroys sweat glands and hair follicles. Muscles, fat, nerves, and bones may be affected. As burns damage nerve endings, so the patient won't feel pain in the area of the burn. Burned skin may be black, white, or red.
There can be various causes for burn, a few of them are mentioned below:
Symptoms depend on the degree, depth, and severity or degree of damage. Burn symptoms include:
Examination of the burn is done to determine the degree or severity. The percentage of the body affected by the burn and its depth is estimated by the rule of nine.
Rule of nine:
Minor burns: These burns cover less than 10% of the body.
Moderate burns: These types of burns cover about 10% of the body.
Severe burns: These burns cover more than 10% of the body.
Pathology
Due to the exposure to heat, chemicals or electricity, the zone of coagulation nearest the heat source is the primary injury. This area undergoes irreversible tissue necrosis at the center.
Ibuprofen, acetaminophen, silver sulfadiazine, silvadine etc.
Note: Medicines should be taken only under the doctor's permission.
Treatment decisions are taken to:
First-degree or minor burns:
Cool compresses should be applied immediately to reduce the swelling and pain. The burnt area is cleaned to prevent infection, dressing is not required. Water-based skin moisturizer may be applied, to help the skin heal.
Second-degree burns:
In case the skin is broken, gently wash by rinsing with a saline solution. If blisters are developed see a doctor.
Third-degree burns:
Third-degree burns can be life-threatening thus requires specialized medical care. Care should be taken to prevent dehydration, prevent infection, remove dead tissue, and cover the wound with skin as soon as possible. Clothing that's stuck to the burn shouldn't be removed and also do not apply cold water. Apply dressing on the burnt area. Skin grafts can be used to replace damaged tissue. In case skin grafts or other surgery is required, the patient is advised to exercise throughout the process of surgery and recovery.
Physiotherapy is an essential part of recovery for burned patients. Physiotherapy treatment includes:
Modalities that are used commonly by the Physiotherapist are:
Transcutaneous Electrical stimulation:
Transcutaneous Electrical stimulation is used to decrease pain and adherence to the underlying scar tissue.
Ultrasound has been used to decrease the pain in the painful joints and also increase the range of motion.
Intermittent compression units and Compression Therapy:
Intermittent compressions units help reduce edema in the extremities. Compression therapy uses tight bandages designed for the patient to put pressure on the burn site and prevent keloids and hypertrophic scars from forming scars as these may limit the range of motion.
Continuous passive motion (CPM) machines:
Continuous passive motion machines are used in patients who need additional range-of-motion treatment for tight areas, and patients following excision of heterotopic ossification.
Splinting:
Splinting can help prevent the formation of skin contracture. This can be helpful during exercises. The splints are designed to control more than one joint while applying pressure over the thick scarred bands. The major areas to concentrate on are hands and other areas requiring splinting are:
Scar Massage:
Scar massage is the process of gently rubbing the scar formed due to burn with a lotion or lubricant. Scar massage can help decrease pain and keep the scarred area flexible.
Skin lubrication:
Skin lubrication helps to keep the skin moist and flexible, it lessens the itchy sensation that accompanies healing burns and also prevents complications that may occur from cracked skin.
Range of motion and stretching exercises:
To maintain the joint range of motion active and passive exercises are given. Thickened bands are formed due to burn scars. For which stretching is also given. Stretching is a slow, sustained stretch technique used for skin contracture. It can be done with traction, splinting, and weights.
Strengthening exercises:
Isometric and isotonic exercises can be given after prolonged inactivity. Endurance and strengthening exercises are given to opposing muscles to prevent the formation of contractures. Cardiovascular fitness programs along with isokinetic strengthening exercises are also recommended.
Psychological support:
The burns patient psychological and emotional support. As burn injury results in depression which can disrupt functional independence. The physiotherapist can teach relaxation exercises that can help sleep peacefully and also decrease stress-related problems.
Select your City to find & connect with our experts regarding Physiotherapy for Burns