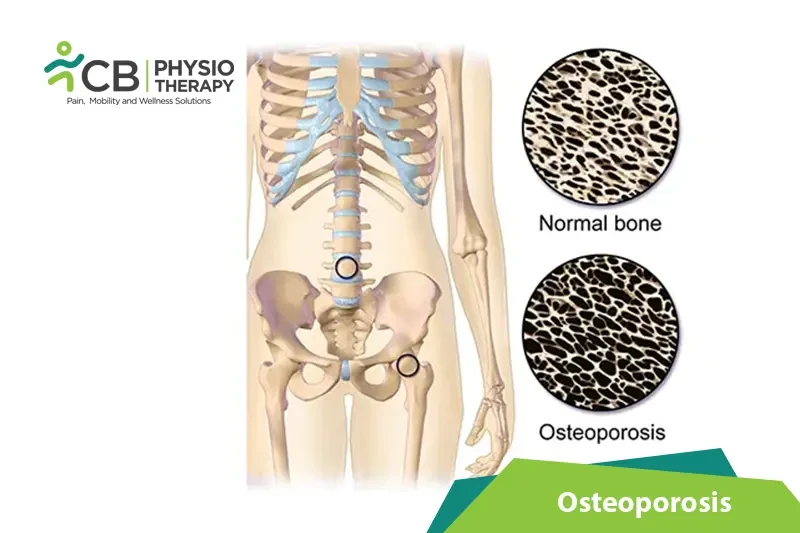
Osteoporosis is a disorder characterized by low bone mass and associated with pathologic fractures. Osteoporotic fractures can affect any part of the skeleton except the skull. Most commonly fractures occur in the distal forearm, proximal femur, thoracic and lumbar vertebrae.
The symptoms of Osteoporosis can be varied depending on the cause and severity, the common symptoms are:
Osteoporosis has no known cause, but there are many factors associated with the disorder. These include:
Pathology:
Osteoporosis is a skeletal disorder causing decreased bone strength and can result in an increased risk of fractures. Throughout the life span, older bone is periodically resorbed by osteoclasts at discrete sites and replaced with new bone made by osteoblasts.
Bone Mineral Density Test:
BMD testing is a safe, fast, and painless method to check whether the patient has osteoporosis or how likely he is to develop it in the future.
DEXA scan:
Dual X-ray absorptiometry test scans (DEXA) of the central skeleton are another diagnostic test for assessing bone mineral density.
Bone density test:
The bone density test uses T-scores. T-scores are relative to how much higher or lower the bone density is compared to that of a healthy 30-year-old adult.
Medication: Bisphosphonates, Denosumab, Selective estrogen receptor modulators (SERMS), Raloxifene, Teriparatide, etc.
Note: Medication should not be taken without the doctor's prescription.
Surgery:
If the patient has a serious osteoporosis fracture, then most likely he needs surgery. The most common locations for osteoporosis-related fractures are the spine, hip, and wrist.
Cryotherapy reduces pain and swellings, which leads to skeletal muscle relaxation and increases joint range of motion.
Thermotherapy or heat therapy improves the symptoms of osteoporosis and can be applied with packs, towels, wax, etc. Heat therapy improves circulation and relaxes the muscles.
Therapeutic ultrasound is commonly used in physiotherapy to provide deep heating to soft tissues in the body. These tissues include muscles, joints, tendons, and ligaments.
Transcutaneous Electrical Stimulation (TENS):
Transcutaneous electrical nerve stimulation helps to relieve pain, maintain or improve functional status, and minimize deformity. TENS is a non-invasive modality in physiotherapy, commonly used to control both acute and chronic pain arising from several conditions.
Orthosis:
An orthosis is also used to protect the spine. These protect the extension of the spine.
Range of motion (ROM):
Range of motion and strengthening exercises can help to maintain the mobility and flexibility of the upper back and core. Fractures and wedging of the vertebra occur due to the increased flexion through the thoracic spine.
Resistance exercises:
As exercises lead to stronger bones, to maintain or improve bone density at the location of the targeted muscle attachments. Physiotherapist designs an appropriate exercise program, which can reduce the risk of falls and related fractures. Exercise programs include the use of gravity resistance exercises, exercise bands e.g, push-ups, single-leg heel raises, squats, lunges, prone trunk extension with a cushion to protect the lowest ribs, and sustained standing positions in neutral spine position.
Loading exercises:
To increase the overall stability and bone strength lifting weights and lower impact exercises can decrease the risk of fracture. People with osteoporosis are usually afraid to perform strengthening exercises, but physiological to improve the function, a load larger than normal must be exposed for strengthening. Bones must be imposed forces greater than those it sustains to improve strength on a day-to-day basis. Weight lifting in the proper alignment can be done. Weight-bearing exercises such stomping, heel drops, dancing, and jogging are also done under the guidance.
Balance and coordination exercises:
Coordination and balance exercises help in reducing the risk of falls. Strengthening the extensor muscles promotes proper posture and balance. When walking through narrow spaces or walking on unstable surfaces, these exercises help to improve balance. Exercising on a wobble board and placing challenges can increase and maintain balance. Exercises should be performed 2 to 3 times a week.
Postural exercises:
These exercises help to prevent structural changes that often accompany osteoporosis, such as thoracic kyphosis. Every osteoporosis exercise program should include chin tucks, scapular retractions, thoracic extensions, and hip extensions.
Agility training:
Agility training and stretching exercises decrease back pain and its related disabilities. These exercises help in the prevention of bone loss for women in menopause and early-stage post-menopausal. Exercises include body-weight and resistive exercises at a high intensity, similar to circuit training. This type of training program is often contraindicated for individuals with low bone mass.
Patients should be advised to avoid exercises that involve repetitive bending and twisting, and strenuous activities, as these increase pressure and friction within the spine, and may lead to fracture. Compression fracture of the spine is also more likely to occur when the abdominal muscles are weak and cannot properly stabilize the spine. High-impact exercises which require forceful twisting motions should also be avoided.
Select your City to find & connect with our experts regarding Physiotherapy for Osteoporosis