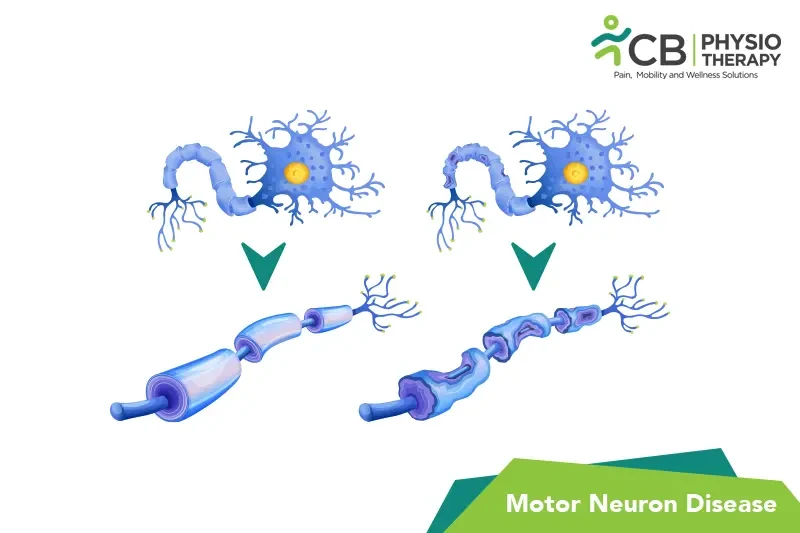
The exact causes of MND are not fully understood, and it can occur sporadically or in a familial form (inherited). Several factors are believed to contribute to its development:
1: Genetic Factors: In some cases, there may be a genetic component to MND, with specific gene mutations linked to the condition.
2: Neuroinflammation: Abnormal immune system responses and inflammation in the nervous system can play a role.
3: Environmental Factors: Some environmental factors, such as exposure to toxins, may increase the risk.
Select your City to find & connect with our experts regarding Physiotherapy for Motor Neuron Disease (mnd)